Classification of Distal Femur Fractures and Their Clinical Relevance
Volume 2 | Issue 1 | Jan-Apr 2016 | Page3-6 |Raja Bhaskara Kanakeshwar, Arun Kamal C, Dheenadayalan J
Author: Raja Bhaskara Kanakeshwar[1], Arun Kamal C[1], Dheenadayalan J[1]
[1]Ganga Hospital, 313, MTP road, Coimbatore , Tamilnadu, India Pin code – 641043
Address of Correspondence
Dr Raja Bhaskara Kanakeshwara
Ganga hospital,313, MTP road, Coimbatore , Tamilnadu, India, Pin code – 641043
Email id – rajalibra299@gmail.com
Abstract
Introduction: Analysis and classifying distal femur fractures is one of the important steps for an orthopaedic surgeon towards a successful outcome in treating these fractures. Few surgeons tried to classify these fractures and we discuss in detail those systems and their clinical relevance . Three classification systems have been discussed below and it has shown the Müller AO classification system remains the ideal classification for these fractures as it is user friendly, easy to document and gives an idea on the prognosis .
Keywords : Distal femur fracture, classification, Müller, AO, Hoffa.
Introduction
To treat a fracture better, we need to understand it better. To understand them better, we need to analyse them better and classify them . Distal femur fractures are often comminuted and intra-articular, and they frequently involve osteoporotic bone, which makes it difficult to reduce them while maintaining joint function and overall limb alignment [1,2]. Hence, classifying them in an appropriate manner which would help surgeons to give a better outcome is of utmost impotance. Unlike proximal femur fractures – which have numerous classifications to describe them – there are only a few systems proposed for distal femur fractures mainly due to the less complex muscular anatomy and vascular anatomy involved between both these regions[3,4,5].
For a classification system to have clinical significance, it must be able to :
1) allow adequate documentation so that a common language is possible to discuss these injuries
2) be ‘user friendly’
3) help in clinical decision making
4) prognosticate the outcome depending on the treatment option [3] .
We shall discuss about the various classification systems described for distal femur fractures and their clinical significance .
Classification of distal femur fractures and their clinical relevance
Classification systems in distal femur fractures :
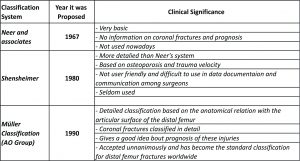
The various classification systems described for distal femur fractures are (Table 1,2) :
1) Neer and associates ( 1967 )
2) Seinsheimer classification ( 1980 )
3) AO Classification – Müller ( 1990 )
Neer and associates classification [ 8 ] :
One of the simpler classification systems of supracondylar femur fractures was that of Neer and associateswhich was described early in 1967 . They subdivided supracondylar- intracondylar femur fractures into three primary categories . The 2nd category had two subdivisions[ 8 ] .
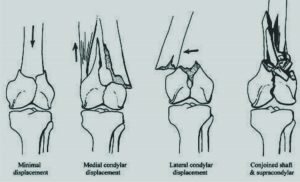
Category I : Minimal displacement
Category II : Displacement of the condyles
A) Medial condyle displacement
B ) Lateral condyle displacement
Category III : Concomitant supracondylar and shaft fractures [Fig 1]
Clinical relevance :
This classification was very basic and did not give much clinical information to the surgeon . No light was thrown upon coronal plane fractures . Moreover , there was no information on the prognosis of these injuries[3]. Hence, this system did not gain much popularity and is seldom used anywhere now among trauma surgeons worldwide .
Seinsheimer classification [9] :
In 1980, Seinsheimer published his system where he classified the fractures of the distal 3.5 inches of the femur into 4 types [9].
Type I : Non-displaced fractures ( less than 2mm displacement )
Type II : Distal metaphyseal fractures ( Extra-articular )
II-A : 2 part fractures
II-B : Communited fractures
Type III : Fractures involving the intercondylar notch in which one or both condyles are separate fragments
Type IV : Intra-articular fractures
IV-A : Medial condyle fracture
IV-B : Lateral condyle fracture
IV-C : Comminuted fractures
Clinical relevance :
Seinsheimer found that the type I and II fracture patients had osteoporosis prior to the injury and they were usually following low energy trauma . On the other end of the spectrum , he found that type IV fractures resulted from high energy trauma[9]. This classification system though it had a better descriptive detail about the fracture pattern , did not become popular as it was not user friendly and provided minimal information on prognosis[3].
AO Classification system – Müller and associates [6,7,80] :
The “Schweizer Arbitsgemenischaft fur Oseosysthesesfragen” Group ( SWISS AO ) , chaired by Müller, through its documentation data centre in Davos brought forward their classification system on distal femur fractures after analysing thousands of these fractures . This system has been found to be easy to use and satisfies all the criteria for an ideal classification [3,8] .
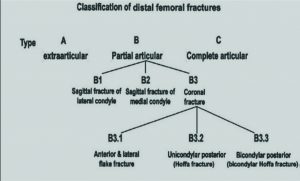
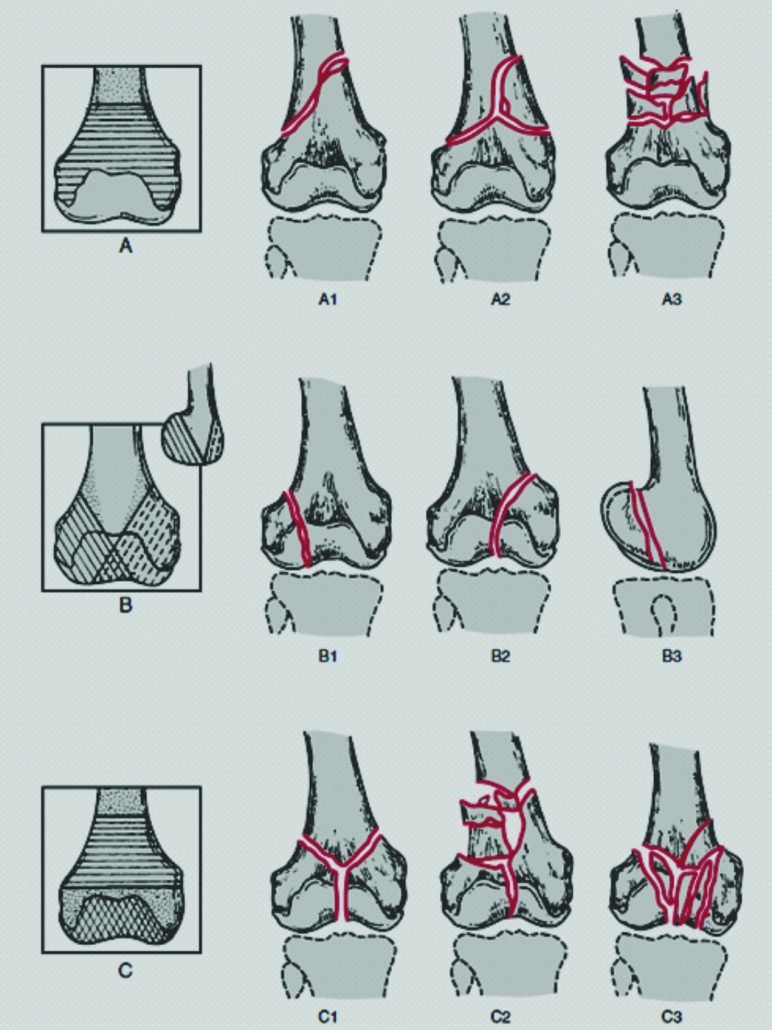
Müller and his colleagues divided these fractures into 3 primary groups [6,8] . Based on the common principles of the AO classification, type A fractures include extra-articular fractures and type B fractures are partial articular fractures, meaning parts of the articular surface remains in contact with the diaphysis of the femur [Fig 2]. Type C fractures include complete articular fractures with both condyles being detached from the diaphysis. The fracture types are further subdivided describing the degree of comminution and other characteristics. Further subdivision of type B fractures includes Bl (sagittal, lateral condyle), B2 (sagittal, medial condyle) and B3 (frontal, Hoffa type). Fracture type C is divided in C1 (articular simple, metaphyseal simple), C2 (articular simple, metaphyseal multifragmentary) and C3 (multifragmentary)[8].
The B3 type fracture – popularly known as ‘Hoffa’s fracture’- has immense clinical signifcance in the outcome following treatment and has been further subdivided into three types [3,8,10] . This type of cornoal fractures of he distal femur are further classified into :
B3.1 – Anterior and lateral flake fracture
B3.2 – Unicondylar Hoffa’s fracture
B3.3 – Bicondylar Hoffa’s fracture
Clinical relevance :
This classification also states that progressing from type A to type C , the severity of the trauma and injury increases whereas the prognosis for a good outcome decreases [3,10,14] . This relation also holds true for the progression from type 1 to type 3 in each group . Communication among surgeons worldwide regarding distal fractures using this system was easy and it was unanimously accepted as the gold standard classification woldwide [3,9].
Regarding the appropriate treatment or surgical option for any particular type of fracture based on the AO Müller classification system , there have been many articles published[11-16] (Table 3) . The final treatment for the patient anyhow needs to be taken by the treating surgeon depending upon many factors including the soft tissue status and the general condition of the patient [16]. A variety of surgical exposures, reduction techniques and various new implants have been developed to treat such fractures and these include intramedullary nailing, screw fixation ,periarticular locked plating and also the LISS ( Less Invasive Stabilization System ) technique [15,16] .
However, in simple fractures compression osteosynthesis should be favoured over bridging osteosynthesis since higher rates of non-unions have been reported for using locking plating for treatment of simple fractures[12].
![Table 3: The recommended Surgical treatment option based upon the type of the Muller's classification is[ 12,13 ] Table 3: The recommended Surgical treatment option based upon the type of the Muller's classification is[ 12,13 ]](http://traumainternational.co.in/wp-content/uploads/2016/05/tab3-300x192.jpg)
Table 3: The recommended Surgical treatment option based upon the type of the Muller’s classification is[ 12,13 ]
Among all the classifications described for distal femur fractures, the Müller AO classification system is the most widely accepted system and is being used worldwide. This classification takes into account the involvement of anatomic region of the distal femur, the energy of the injury and also prognosticates the outcome . It has a high inter-observer reliability and validity. Being user friendly and also serving as a common language among surgeons worldwide to discuss distal femur fractures, this classification is the one of choice for treating these fractures.
References
1. Gwathmey FW Jr, Jones-Quaidoo SM, Kahler D, Hurwitz S, Cui Q. Distal femoral fractures: current concepts. J Am Acad Orthop Surg. 2010 Oct;18(10):597-607.
2. Everhart JS, Chaudhari AM, Flanigan DC. Creation of a simple distal femur morphology classification system. J Orthop Res. 2015 Nov 17.
3. Krettek C, Schandelmaier P, Richter M, Tscherne H. [Distal femoral fractures].Swiss Surg. 1998;(6):263-78.
4. Martinet O, Cordey J, Harder Y, Maier A, Bühler M, Barraud GE. The epidemiology of fractures of the distal femur. Injury. 2000 Sep;31 Suppl 3:C62-3.
5. Mu¨ller, M.E.; Allgo¨wer, M.; Schneider, R.; Willenegger, H. Manual of Internal Fixation, 3rd ed. New York, Springer-Verlag, 1991.
6. Mu¨ller, M.E.; Nazarian, S.; Koch, P. 1987. Classification AO des Fractures. Springer-Verlag New York,
7. Mu¨ller, M.E.; Nazarian, S.; Koch, P.; Schatzker, J. The Comprehensive Classification of Fractures of Long Bones. New York, Springer-Verlag, 1990.
8. Neer, C.S.; Grantham, S.A.; Shelton, M.L. Supracondylar fracture of the adult femur. A study of one hundred and ten cases. J Bone Joint Surg Am 49:591–613, 1967.
9. Seinsheimer, F. Fractures of the distal femur. Clin Orthop 153:169–179, 1980.
10. Stover M.: Distal femoral fractures: current treatment, results and problems. Injury, 32 (Suppl. 3): SC3-13, 2001
11. ZLOWODZKI M, BHANDARI M, MAREK DJ, COLE PA, KREGOR PJ. Operative treatment of acute distal femur fractures: systematic review of 2 comparative studies and 45 case series (1989 to 2005). J. Orthop. Trauma, 20: 366-371, 2006
12. LIU, E., TAO, R., CAO, Y., WANG, Y., ZHOU, Z., WANG, H., et al.: The role of LISS (less invasive stabilisation system) in the treatment of peri-knee fractures. Injury, 40: 1187-1194, 2009.
13. SHAHCHERAGHI, G. H., DOROODCHI, H. R.: Supracondylar fracture of the femur: closed or open reduction? J. Trauma, 34: 499-502, 1993.
14. Bel JC, Court C, Cogan A, Chantelot C, Piétu G, Vandenbussche E; SoFCOT. Unicondylar fractures of the distal femur. Orthop Traumatol Surg Res. 2014 Dec;100(8):873-7.
15. Arastu MH, Kokke MC, Duffy PJ, Korley RE, Buckley RE. Coronal plane partial articular fractures of the distal femoral condyle: current concepts in management. Bone Joint J. 2013 Sep;95-B(9):1165-71.
16. Pritchett, J.W. Supracondylar fractures of the femur. Clin Orthop 184:173–177, 1984.
| How to Cite this article: Raja BK, Arun KC, Dheenadayalan J. Classification of distal femur fractures and their clinical relevance. Trauma International Jan-Apr 2016;2(1):3-6. |