Definitive Management of Pelvic Fractures
Vol 3 | Issue 1 | Jan – Apr 2017 | page:17-23 | Vivek Trikha, Saubhik Das.
Author: Vivek Trikha [1], Saubhik Das [1]
[1] Department of Orthopaedics, AIIMS & JPNATC, New Delhi, India..Address of Correspondence:
Address of Correspondence
Dr. Vivek Trikha,
Department of Orthopaedics, AIIMS & JPNATC, New Delhi, India.
E-mail: vivektrikha@gmail.com
Abstract
Pelvic fractures constitute one of the most severe orthopedic injuries causing significant mortality and morbidity. It poses a diagnostic and therapeutic challenge to orthopedic surgeons. Once the patient is resuscitated and stabilized, definitive reconstruction of pelvic fracture is planned. Management depends on patient’s physiologic status, fracture characteristics, and associated injuries. Early fixation has proven to be beneficial. Our paper focuses on definitive management of pelvic fracture, with emphasis on surgical approach, fixation methods and principles.
Keywords: Complication, definitive management, functional outcome, pelvic fracture.
Introduction
Pelvic fractures constitute one of the most severe orthopaedic injuries causing significant mortality and morbidity. Pelvic fractures can either be stable fractures resulting from low energy trauma, for example iliac wing or isolated ramus fractures, or more importantly, unstable fractures from high energy injury. Most of these results from road traffic accidents, falls from height, or occasionally, work place crushing accidents, and are often associated with other injuries like injuries of the abdomen or pelvic viscera, urogenital injuries, neurovascular injuries in the pelvis retroperitoneal region and other lower limb fractures. Once patient is optimised and fully resuscitated with haemorrhage control and temporary pelvic stabilisation, definitive surgical fixation is contemplated to address pelvic instability and improve long term outcomes. Surgical decision making is a complex process and challenging even to the most experienced orthopaedic surgeons.
Classification
There are various classifications proposed for the pelvis fracture like Tile’s, Young- Burgess and AO/OTA Classification. The classification described by Young and Burgess is widely followed [1]. It reflects the mechanism of injury as well as the degree of injury. Based on mechanism, pelvic fractures are classified into four types- anteroposterior compression (APC), lateral compression (LC), vertical shear (VS) and combined type in this classification
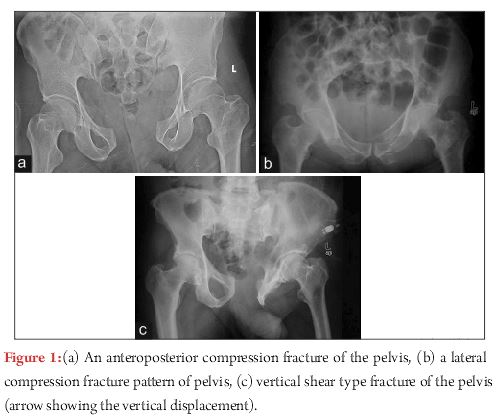
1) Antero-posterior compression (APC, Fig-1A):
Antero-posterior direct compression force leads to diastasis of the symphysis pubis or vertical rami fractures anteriorly. In type I injury, diastasis of pubic symphysis is typically <2.5cmand posterior pelvic ligaments (anterior and posterior sacroiliac, sacrotuberous, and sacrospinous) are intact. With greater force, injuries progress to APC type II, which is characterised by the symphyseal diastasis>2.5cm, with anterior opening of sacroiliac(SI) joint. There is disruption of anterior sacroiliac (SI), sacrotuberous(ST), and sacrospinous(SSp) ligaments; however the posterior SI ligaments remain intact. With still greater force, there is complete disruption of anterior and posterior SI ligaments, producing unstable SI joint and APC type III pattern.
2) Lateral compression (LC, Fig-1B):
Lateral compression injuries are the most frequently encountered pattern. They result from side impact during motor vehicle collision or fall from height. Anterior injury typically demonstrates transverse pubic rami fractures. In LC type I injuries, there is sacral impaction fracture posteriorly. LC type II pattern has iliac wing or crescent fracture posteriorly. LC type III injuries (‘windswept pelvis’) are characterised by composite injury of LC I or LC II on side of impact, with contralateral open book (APC) injury.
3) Vertical Shear (VS, Fig-1C):
A vertically directed force results in disruption of both anterior and posterior elements, with vertical displacement of one hemipelvis with respect to the other. A fracture of the transverse process of L5 vertebra is often a tell-tale sign of such an injury.
4) Combined:
A combination of the above mechanisms of injury is classified as “combined” pattern. It usually involves the LC and the VS pattern of injury.
Definitive management
Definitive management of pelvic fractures is contemplated after patient is optimised and conducive for surgical intervention. Pelvic radiographs (anteroposterior, inlet, outlet view), CT scan with 3D reconstruction are carefully evaluated to define fracture configurations. Dynamic stress view is often sought for elucidation of occult instability.
Some basic tenets of pelvic fracture management are
1. Integrity of posterior pelvic ring is most critical for overall pelvic stability.
2. If there is disruption of posterior pelvic ring (sacral fracture, SI joint disruption, iliac wing or crescent fractures), with vertical instability of hemipelvis, posterior fixation should ideally be augmented by some form of anterior fixation (ORIF/ external fixator) to restore stability [2].
3. Classically, fixation should proceed from posterior to anterior [3]. However, controversy surrounds this approach, with some advocating front first approach [4].
Indications for surgery
APC type I fracture is generally stable pattern (symphyseal widening< 2.5 cm), and usually treated nonoperatively with good results. Caution must be exercised to differentiate APC type I injury from APC type II injury. If concern exists, dynamic stress view and/or examination under anaesthesia must be performed to elucidate occult instability which necessitates fixation. Similarly, LC type I fractures are usually treated nonoperatively. Whereas, APC and LC type II and III fractures are rotationally unstable,which require surgical stabilisation. In vertical shear (VS) injury, there is complete disruption of ligamentous support with cephalad migration of hemipelvis. Surgical stabilisation is required in all VS injuries.
Tworare LC variants deserve special mention; locked symphysis and tilt fracture [5]. During lateral compression, intact pubis can cross midline and get entrapped into the obturator foramen. If closed reduction is unsuccessful and pelvic instability persists, open reduction and stabilisation is necessary. Similarly in tilt fracture, superior ramus is pushed posteriorly and inferiorly into the perineum. This can lead to dyspareunia in female patients. Surgical management is often considered to reduce this fracture and avoid later dyspareunia.
Timing for definitive fixation
Optimal time frame for definitive surgical stabilisation has not been clearly defined. There is recent trend towards acute surgical stabilisation; time frame varies in literature from as early as less than 24 hours to less than one week after injury [6, 7].Our preference is to fix most of the fractures within the first one week after injury once patient is optimised, albeit early fixation is associated with risk of bleeding and potential for second hit in multiply injured patients.Proponents for early fixation cites several advantages; improved fracture reduction, early mobilisation and pain relief, less risk of pulmonary complication and deep vein thrombosis, shorter hospital stay [7]. However, treatment should be individualised and several factors should be kept in mind to decide optimal time for surgery such as; patient’s haemodynamic status and co morbidities, associated injuries, and soft tissue condition etc.
Option for surgical fixation and approach for anterior pelvic ring
1. External fixation:External fixator has proved to be a valuable tool for emergent as well as definitive management of pelvic fractures. This device usually is employed during:
1. As a temporizing measure during Emergent stabilisation of unstable pelvic injury in haemodynamically unstable patient.
2. As a definitive method of fixation of anterior pelvic ring when internal fixation is precluded (extraperitoneal bladder rupture, or when open laparotomy wound poses potential risk of infection of internal fixation).
3. Occasionally as a supplemental fixation following posterior pelvic ring stabilisation.
Various external fixator configurations have been described for the traditional anterior external fixator. Although they are equally effective in resisting rotational forces, none of these fixators are sufficient enough to stabilise vertically unstable pelvis [8]. Moreover, anterior frame require intact posterior hinge to close and stabilise pubic diastasis.
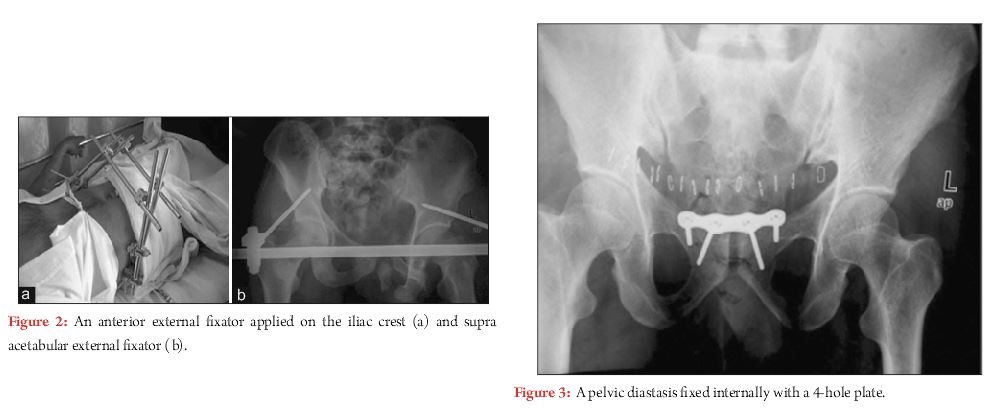
Two sites for pin placement for anterior external fixator have been described; into the iliac crest (Fig. 2-A), and into the dense supraacetabular bone (Fig. 2-B). Compared to iliac crest pins, supraacetabular pin placement requires precise technique and fluoroscopic guidance. Pins are directed from anteroinferior iliac spine (AIIS) towards sciatic buttress. Starting point and interosseous path of screw between inner and outer table of pelvis is obtained by obturator oblique outlet view. Additionally, iliac oblique inlet view demonstrates trajectory of screw over greater sciatic notch and hip joint towards sciatic buttress. Recently internal external fixator using pedicle screws in place of supraacetabular pins(INFIX) [9], andplate internal fixator [10] have been described. Better biomechanical advantage and avoidance of pin site complications are potential advantages of these techniques.
2.Internal fixation
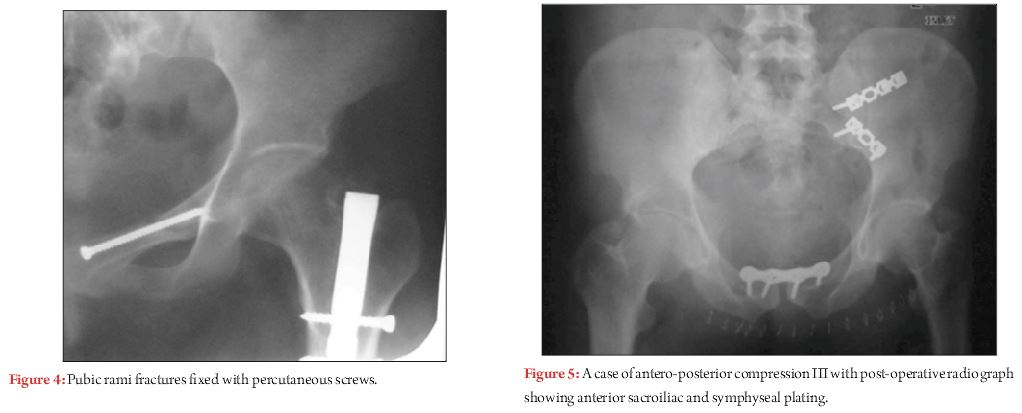
Pfannenstiel approach is the mainstay for internal fixation of anterior pelvic ring (Fig. 3). Transverse incision is placed twofingerbreadths above symphysis pubis. Usually longitudinal incision is made into linea alba. Very often, rectus abdominis is torn off at least on one side, this allow easy access without disturbing rectus insertion much. Sometimes fixation of rami fracture is considered especially in rotationally and/ or vertically unstable pelvic injury with significant soft tissue damage, as an adjunct to posterior fixation. In most of the cases, rami fractures can be treated nonoperatively, as intact periosteal hinge and inguinal ligament provide favourable biological and mechanical environment for healing. Options for internal fixation of rami fractures include; ORIF with plating, percutaneous screw(antegrade or retrograde). For ORIF of rami factures, Pfannenstiel incision is used and subperiosteal dissection is carried further laterally up to pelvic brim, or formal Stoppa’s approach can be performed. Caution should be taken to avoid injury to corona mortis (anastomosis between external iliac and obturator vessels), which should be protected and ligated.To avoid extensive surgical dissection, many surgeons are adopting percutaneous fixation with antegrade or retrograde screw (Fig. 4). Biomechanically retrograde ramus screw is found to be as effective as plating. Screw position and technique largely depends upon fracture configuration, location, associated soft tissue injury, and body habitus of patient. In general, antegrade screw (from supra-acetabular area and directed medially towards symphysis pubis) is used for rami fractures located in middle or lateral third, and in obese patient. Whereas retrograde screw (from pubic tubercle and directed laterally above the acetabulum) is preferred for medially based fractures [11]. Surgeon well versed with this technique and proper fluoroscopic view is paramount for accurate screw placement. Complications most often arise due to improper trajectory of screw leading to injury to adjacent structure such as; external iliac vasculature, corona mortis, bladder, urethra, and penetration into hip joint.
Option for surgical fixation and approach for posterior pelvic ring:
1. Percutaneous iliosacral screw:
Percutaneous iliosacral screw is increasingly being used for SI joint dislocation as well as some sacral fractures. Minimally invasive nature, and equivalent biomechanical properties compared to transiliac fixation and anterior SI plating, has led to the popularity of this method [12]. Well trained pelvic surgeon with in depth knowledge and orientation of anatomic as well as radiographic landmarks, is critical for proper execution of the procedure. Inlet, outlet and lateral sacral radiographic view is paramount to ensure safe trajectory of screw. Safe corridor for screw placement is marked by identification of radiographic landmarks such as; iliac cortical density corresponding to sacral ala on which L5 nerve rests, anterior cortex of sacral promontory where great vessels lie, posterior border of S1 corresponding to anterior aspect of sacral canal, S1 foramen. Detailed evaluation of preoperative x ray and CT scan with 3D reconstruction is paramount to identify sacral dysmorphism and spinal abnormalities, if any, that could alter placement of screw to avoid inadvertent injury to nearby structures. Recently, computer navigation and 3D imaging have been found useful for this procedure [13].
2. Open reduction and fixation:
SI joint dislocation requiring open reduction can be accessed through posterior or anterior approach. For posterior approach, patient is positioned prone on radiolucent table and paramedian incision is used. Clamp placement is easier from posterior approach. However, direct visualisation of fracture reduction is difficult. Palpation of anterior SI joint through greater sciatic notch helps to ensure anatomic reduction. Fixation options include percutaneous iliosacral screw, iliac bars, tension band plating. For SI joint dislocation requiring anterior approach, lateral window of ilioinguinal approach is employed. Fixation is achieved by anterior SI plating, percutaneous iliosacral screw, or combination of both; no biomechanical differences has been found between these. Due to proximity of L5 nerve over sacral ala, only one hole of the plate can be placed safely over sacral ala. Therefore two plates at an angle of less than 90° to each other are necessary to gain control of injured SI joint. Safe placement of reduction clamp and fixation device is imperative to avoid injury to L5 nerve.
For iliac wing fracture, anterior or posterior approach is used, whichever is deemed necessary. Two plates are generally required to neutralise deforming forces; one along iliac crest and pelvic brim (anterior approach), and sciatic buttress along with iliac crest (posterior approach). Additionally, lag screw along the crest can be employed to achieve compression.
Management of specific injury pattern:
1. Antero-posterior compression(APC) injury:
Rotationally unstable APC type II and III injuries necessitate surgical stabilisation. After exposure through Pfannenstiel type incision, there are several methods to achieve and maintain reduction. Internal rotation and taping of lower extremities along with Weber reduction clamp with its tines placed on each pubic tubercle can assist in reduction. Additionally, Farabeuf or Jungbluth clamp, which utilizes 3.5 or 4.5 mm screws, also assist in reduction. They are particularly useful to correct associated sagittal rotation (flexion/extension), and posterior translation of hemipelvis, often associated with posterior ring injury. Controversy surrounds concerning the plate configuration for symphyseal diastasis. Previously two hole plate have been advocated, which theoretically maintain physiologic motion at symphysis pubis. However, high failure and malunion rate with two hole construct prompted pelvic surgeons to use multi-hole construct with at least 2 point of fixation on either side of symphysis [14]. Our preference is to use multi-hole 3.5 mm symphyseal specific or pelvic reconstruction plate with at least 2 point of nonlocking fixation on either side (Fig. 3). Although locking plate could be beneficial in osteoporotic bone, their superiority over non-locked device is questionable [15]. Proper screw trajectory should be maintained to avoid inadvertent injury to bladder, which can be ascertained by finger palpation of posterior aspect of pubis.
In APC type II injury, need for posterior fixation is a point of debate. A recent literature tried to address this issue bysub classifying APC type II injury. In type IIa subtype, posterior sacroiliac (SI) ligaments are intact, and anterior fixation alone is sufficient. In type IIb subtype, posterior SI ligaments are attenuated (not disrupted), which contribute to the sagittal plane instability of hemipelvis. On dynamic stress view, sagittal plane displacement of hemipelvis > 1 cm signifies unstable injury, and necessitates supplemental posterior fixation via iliosacral screw [16]. Both anterior and posterior stabilisation is deemed necessary for APC type III injury (Fig. 5). Controversy exists regarding sequence of fixation. Posterior ringstabilisation followed by anterior ring is the classically described method of fixation. However, many authors have reported favourable outcome with the reverse sequence progressing anterior to posterior [4, 17]. It is imperative to keep in mind that proper reduction of anterior ring is paramount to gain control and anatomic restoration of posterior ring in this method.
2. Lateral compression (LC) injury:
LC type II injury involves either fracture through entire ilium, or crescent fracture posteriorly, associated with anterior rami fractures. In crescent fractures, the fracture goes through the iliac wing and into the SI joint with substantial disruption of SI joint ligament complex, yielding rotationally unstable hemipelvis [18]. The crescent fragment comprising Postero superior iliac spine (PSIS) and Postero inferior iliac spine (PIIS) remains attached to sacrum by posterior and interosseous SI ligaments. Surgical management is deemed necessary for this uncommon injury. Day et al. [19]proposed a functional classification of crescent fracture and suggested management algorithm, which can aid surgeons in deciding appropriate treatment. Type I fracture involves large crescent fragment with fracture line involving anterior third of SI joint. This can be addressed by lateral window of ilioinguinal approach with plate fixation. Type II fracture comprising intermediate size fragment with fracture line exiting through mid third of SI joint, can be addressed by posterior approach. Fixation by lag screw from PIIS towards sciatic buttress, parallel to SI joint, with supplemental plate fixation yield stable construct. Type III fracture involve most but not all of the SI joint with fracture line exiting through posterior part of SI joint. Crescent fragment is small in size. This is amenable to closed reduction with percutaneous iliosacral screw fixation. In case of delayed presentation with unsuccessful closed reduction, anterior approach with plate fixation can be considered.
LC type III injury with ‘windswept’ pelvis can be managed in line of APC and LC injury in combination. Evaluation of fracture configuration and instability pattern can aid in deciding systematic management strategy.
3. Vertical shear(VS) injury and sacral fracture:
VS injuries are very unstable pattern. If posterior component is pure SI joint dislocation, then anatomic reduction and iliosacral screw fixation is performed. Anterior fixation should be performed as an adjunct to posterior fixation to neutralise potential deforming forces (Fig. 6).
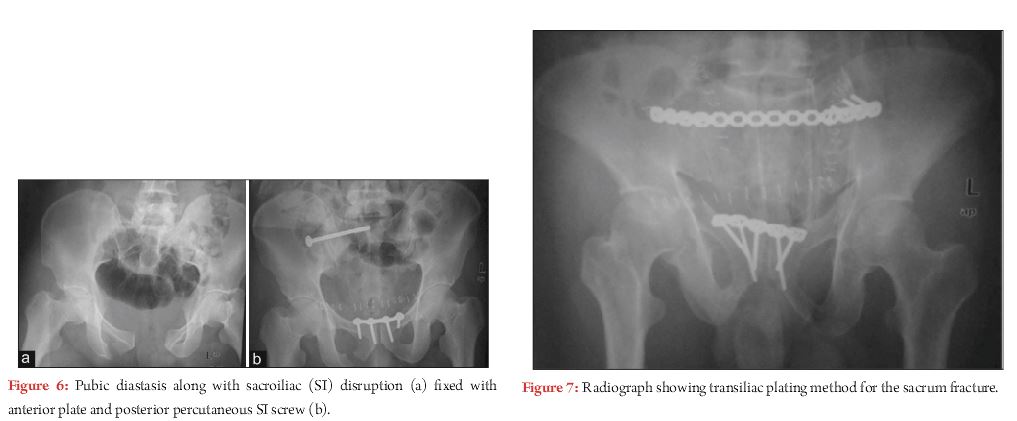
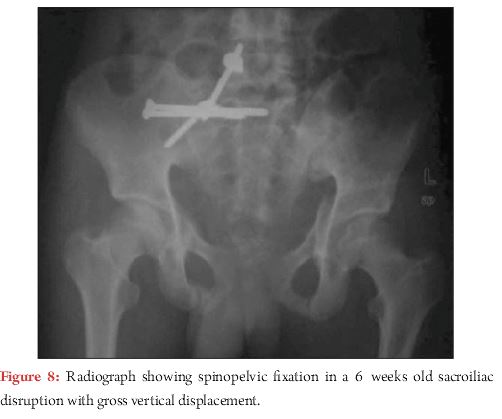
Concern arises regarding inadequate screw purchase in transforaminal, comminuted sacral fractures. Transsacral fixation with partially or fully treaded screw has proved to be beneficial demonstrating favourable results, especially with use of locking nuts [20]. Other fixation options include iliac bar, transsacral plating, spino-pelvic construct (Fig. 7 and 8). Substantial vertical instability with comminuted sacral fracture, spino-pelvic dissociation, disruption of L5-S1 facets, and late cases of VS injury with sacral fracture can be addressed by spino-pelvic fixation. Triangular osteosynthesis refers to spino-pelvic fixation combined with iliosacral screw [21].Literature supports superior biomechanical properties of these constructs compared to iliosacral screw (Fig. 8) [22].
4. Open pelvic injury:
If the pelvic fracture has a direct communication with the outside environment it is open in nature. It may communicate to the skin from the abdomen, scrotum, buttock or back, rectum or vagina. Its incidence is less than 5% of all pelvic injuries however, the mortality figures range from 5-45%, generally around 25%. Compounding, internal or external, worsens the prognosis [23]. This injury is the result of a very high energy impact and invariably has associated injuries. Any external wound on the lower abdomen, pelvis, scrotum or the genital region should be considered to be communicating with the pelvis injury until proven otherwise. Open fractures require provisional pelvic stabilisation with fixator, thorough wound debridement, and suprapubic catheterisation or diversion colostomy. A multidisciplinary approach is warranted, and communication with concerned specialities is paramount in placing diverting colostomy and suprapubic catheter as far as possible from planned surgical site to avoid potential contamination of internal fixation.
A Morel-Lavallee lesion is an equally sinister injury pattern [24]. It is described as an internal degloving injury around the hip when the skin and the subcutaneous tissues are traumatically separated from the underlying muscle fascia, fatty and soft tissue. A sizable amount of fluid may collect in the closed space which is characteristic of this lesion. It might be missed and the fracture treated as a closed injury with disastrous consequences. It needs a thorough open debridement with external fixation or percutaneous drainage in acute stage. Percutaneous fixation, if possible, can be done. Vacuum assisted closure has a role in the management of such wounds [25]. In such cases external fixation forms the mainstay of treatment initially, which may be converted to definitive stabilization once the soft tissue stabilizes.
Complications and Outcome:
In an analysis of more than 63 thousand patients, the odds ratio for mortality associated with a pelvic fracture was found to be 2.0, which were similar to that for an abdominal injury [26].Haemorrhage and closed head injury constitute the two most common causes of early mortality. Sepsis and multi organ failure are the major causes of late mortality. Besides the early and late mortality, pelvis fractures are also associated with late morbidity. The stable fractures usually do well and cause minimal disability while the unstable fractures have a higher rate of deformity and disability.
Pain is an important cause of morbidity after pelvic fractures. Its incidence is highest in patients with unstable pelvic injury and major pelvic disruptions. If the major weight bearing arch of pelvis i.e., the posterior pelvic element is displaced and not reduced, it may lead to malunion, non-union or osteoarthritis of the SI joint. This may cause disabling pelvic pain which is most common with combined or vertical shear type of fracture. It has been postulated that if the residual displacement is more than 1 cm, nearly 70% of patients shall have severe pain with abnormal function. Neurological injury is most common after unstable vertical shear fractures, posterior pelvic injuries and Denis type III sacral fractures. Careful evaluation and documentation is essential to look for the sensory deficits around perineum and sphincter function.
The incidence of genitourinary injury in pelvic fractures has been reported to be 4.6%. It is twice as common in males as in females. Patients with genitourinary injury have greater ICU stay and increased mortality rates as compared to those without genitourinary injury [27]. Posterior pelvic injuries are involved in the ejaculatory disturbances while the anterior injuries, especially the diastasis, cause the erectile dysfunctions. In females also, dyspareunia is common after diastasis or rami fractures.
Evaluation of outcome following pelvic fracture fixation is difficult to assess because of diversity of fracture pattern and treatment options, associated injuries, and lack of validated outcome measures. Literature unveils that posterior ring stabilisation with less than 1 cm of displacementproduces favourable long term outcome, especially in pure SI joint dislocation [28, 29]. Moreover bony injury of posterior ring is thought to do better as compared to ligamentous disruption, because of bone to bone healing is believed to restore strength and stability [30].However, there is no reference standard in literature what constitutes an accurate reduction, which is supported by the fact that despite near normal anatomic reduction, substantial proportions of patients continue to have chronic pelvic pain and some persistent impairment in longterm [31-34].A recent prospective observational study concluded that Two years after surgical treatment of pelvic ring fractures, patients reported substantially lower quality of life for both physical and mental domains, when compared with a reference population, even when radiological and clinical outcomes were considered favourable [35].
Conclusion
Pelvic fracture management is a complex decision making process which poses a therapeutic challenge to even most experienced orthopaedic surgeons. APC and LC type I injuries are successfully treated nonoperatively. Whereas APC and LC type II and III injuries require operative treatment with anterior and/or posterior fixation depending on fracture geometry and instability pattern. VS injuries are most unstable pattern requiring operative stabilisation. In general, anatomic restoration of posterior pelvic ring is paramount, which often is supplemented by anterior fixation to yield stable pelvic construct. Open pelvic fractures necessitate multidisciplinary approach with expeditious wound management, provisional pelvic stabilisation.
References
1. Burgess AR, Eastridge BJ, Young JW, et al. Pelvic ring disruptions:effective classification system and treatment protocols. J Trauma1990;30:848–56.
2. Stocks GW, Gabel GT, Noble PC, et al. Anterior and posterior internal fixation of vertical shear fractures of the pelvis. J Orthop Res. 1991;9:237–245.
3. Lefaivre KA, Starr AJ, Reinert CM. Reduction of displaced pelvic ring disruptions using a pelvic reduction frame. J Orthop Trauma. 2009;23:299–308.
4. Krappinger D, Larndorfer R, Struve P, et al. Minimally invasive transiliac plate osteosynthesis for type C injuries of the pelvic ring: A clinical and radiological follow-up. J Orthop Trauma. 2007;21:595–602.
5. Langford JR1, Burgess AR, Liporace FA, Haidukewych GJ. Pelvic fractures: part 2. Contemporary indications and techniques for definitive surgical management.J Am Acad Orthop Surg. 2013 Aug;21(8):458-68.
6. Connor GS, McGwin Jr G, Maclennan PA, Alonso JE, Rue 3rd LW. Early versus delayed fixation of pelvic ring fractures. Am Surg. 2003; 69(12): 1019-1023 (discussion 1023-4).
7. Vallier HA, Cureton BA, Ekstein C, Oldenburg FP, Wilber JH. Early definitive stabilization of unstable pelvis and acetabulum fractures reduces morbidity. J Trauma. 2010;69 (3):677–684.
8. Tile M. Acute pelvic fractures: II. Principles of management. J Am Acad Orthop Surg. 1996;4(3):152–161.
9. Vaidya R, Colen R, Vigdorchik J, Tonnos F, Sethi A: Treatment of unstable pelvic ring injuries with an internal anterior fixator and posterior fixation: Initial clinical series. J Orthop Trauma 2012;26(1):1-8.
10. Cole PA, Gauger EM, Anavian J, Ly TV, Morgan RA, Heddings AA: Anterior pelvic external fixator versus subcutaneous internal fixator in the treatment of anterior ring pelvic fractures. J Orthop Trauma 2012;26(5): 269-277.
11. Starr AJ, Nakatani T, Reinert CM, et al. Superior pubic ramus fractures fixed withpercutaneous screws: What predicts fixation failure? J Orthop Trauma. 2008;22:81–87.
12. Yinger K, Scalise J, Olsen SA, et al. Biomechanical comparison of posterior pelvic ring fixation. J Orthop Trauma. 2003;17:481–487.
13. Zwingmann J, Konrad G, Mehlhorn AT, et al. Percutaneous iliosacral screw insertion: Malpositioning and revision rate of screws with regards to application technique (navigated vs. conventional). J Trauma. 2010;69:1501–1506.
14. Sagi HC, Papp S. Comparative and clinical and radiographic outcome of two-hole and multi-hole symphyseal plating. J Orthop Trauma. 2008 Jul; 22(6): 373-8.
15. Grimshaw CS, Bledsoe JG, Moed BR. Locked versus standard unlocked plating of the pubic symphysis: A cadaver biomechanical study. J Orthop Trauma. 2012;26:402-06.
16. Sagi HC, Coniglione FM, Stanford JH: Examination under anesthetic for occult pelvic ring instability. J Orthop Trauma 2011;25(9):529-536.
17. Mullis BH, Sagi HC: Minimum 1-year follow-up for patients with vertical shear sacroiliac joint dislocations treated with iliosacral screws: Does joint ankylosis or anatomic reduction contribute to functional outcome? J Orthop Trauma;22(5):293-298.
18. Borrelli J Jr, Koval KJ, Helfet DL: Operative stabilization of fracture dislocations of the sacroiliac joint. Clin Orthop Relat Res 1996;329:141-146.
19. Day AC, Kinmont C, Bircher MD, Kumar S: Crescent fracture-dislocation of the sacroiliac joint: A functional classification. J Bone Joint Surg Br 2007;89(5):651-658.
20. Tabaie SA, Bledsoe JG, Moed BR:Biomechanical comparison of standardiliosacral screw fixation to transsacrallocked screw fixation in a Type C – ZoneII pelvic fracture model.J Orthop Trauma. 2013 Sep;27(9):521-6.
21. Sagi HC: Technical aspects and recommended treatment algorithms in triangular osteosynthesis and Spinopelvic fixation for vertical shear transforaminal sacral fractures. J Orthop Trauma 2009; 23(5):354-360.
22. Schildhauer TA, Ledoux WR, Chapman JR, Henley MB, Tencer AF, Routt ML Jr: Triangular osteosynthesis and iliosacral screw fixation for unstable sacral fractures: A cadaveric and biomechanical evaluation under cyclic loads. J Orthop Trauma 2003;17(1):22- 31.
23. Brenneman FD, Katyal D, Boulanger BR, Tile M, Redelmeier DA. Longterm
outcomes in open pelvic fractures. J Trauma 1997;42:773–7.
24. Hak DJ, Olson SA, Matta JM. Diagnosis and management of closed internal degloving injuries associated with pelvic and acetabular fractures: the Morel-Lavallée lesion. J Trauma 1997;42:1046–51.
25. Labler L, Trentz O. The use of vacuum assisted closure (VAC) in soft tissue injuries after high energy pelvic trauma. Langenbecks Arch Surg 2007;392:601–9.
26. Sathy AK, Starr AJ, Smith WR, et al. The effect of pelvic fracture on mortality after trauma: an analysis of 63,000 trauma patients. J Bone Joint Surg Am 2009;91:2803–10.
27. Bjurlin MA, Fantus RJ, Mellett MM, Goble SM. Genitourinary injuries in pelvic fracture morbidity and mortality using the National Trauma Data Bank. J Trauma 2009;67:1033–9.
28. Dujardin FH, Hossenbaccus M, Duparc F, et al. Long-term functional prognosis of posterior injuries in high-energy pelvic disruption. J Orthop Trauma. 1998;12:145–150.
29. Hoffman MF, Jones CB, Sietsma DL. Persistent impairment after surgically treated lateral compression pelvic injury. Clin Orthop Relat Res. 2012Aug; 470(8): 2161-72.
30. Cole JD, Blum DA, Ansel LJ. Outcome after fixation of unstable posterior pelvic ringinjuries. Clin Orthop Relat Res. 1996;329:160–179.
31. Oliver CW, Twaddle B, Agel J, Routt ML Jr. Outcome after pelvic ring fractures: evaluation using the medical outcomes short form SF-36. Injury 1996;27:635– 41.
32. Pohlemann T, Gansslen A, Schellwald O, et al. Outcome after pelvicring injuries. Injury 1996;27(suppl 2):B31– 8.
33. Van den Bosch EW, Van der Kleyn, Hogervorst M, et al. Functional outcome of internal fixation for pelvic ring fractures. J Trauma. 1999;47:365–371.
34. Kabak S, Halici M, Tuncel M, et al. Functional outcome of open reduction and internal fixation for completely unstable pelvic ring fractures (type C): A report of 40 cases. J Orthop Trauma. 2003;17:555–562.
35. Borg T, Berg P, Fugl-Meyer K, Larsson S: Health-related quality of life and life satisfaction in patients following surgically treated pelvic ring fractures: A prospective observational study with two years follow-up. Injury 2010;41(4):400-404.
| How to Cite this article: Trikha V, Das S. Definitive Management of Pelvic Fractures. Trauma International Jan-Apr 2017;3(1):17-23. . |